
This article aims to explain the details of Toxoplasmosis, a parasitic disease that can affect both cats and humans. There are many misunderstandings about this infection, and this will provide a simple, clear explanation about Toxoplasmosis for cat owners.
Quick Overview: Toxoplasmosis in Cats
 Other Names: Toxoplasma gondii
Other Names: Toxoplasma gondii
 Common Symptoms: Many cats are asymptomatic. Ill cats may show signs including lethargy, fever, yellowing of the gums and skin (jaundice), vision loss, behavior changes, lack of coordination, seizures, neck pain.
Common Symptoms: Many cats are asymptomatic. Ill cats may show signs including lethargy, fever, yellowing of the gums and skin (jaundice), vision loss, behavior changes, lack of coordination, seizures, neck pain.
 Diagnosis: Antibody titer testing can help determine latent vs. recent infection that may correlate to signs of disease. Tissue biopsy samples and cerebrospinal fluid (CSF) samples may also utilized.
Diagnosis: Antibody titer testing can help determine latent vs. recent infection that may correlate to signs of disease. Tissue biopsy samples and cerebrospinal fluid (CSF) samples may also utilized.
 Requires Ongoing Medication: No
Requires Ongoing Medication: No
 Vaccine Available: No
Vaccine Available: No
 Treatment Options: Many cats who are active carriers but who are not ill don't require treatment. A course of a few weeks of a specific antibiotic combined with other therapies may be used for clinically ill cats.
Treatment Options: Many cats who are active carriers but who are not ill don't require treatment. A course of a few weeks of a specific antibiotic combined with other therapies may be used for clinically ill cats.
 Home Remedies: None. Cats can contract toxoplasmosis through hunting birds and rodents, and eating undercooked food. Preventing outdoor exposure, hunting, and feeding raw food can reduce risk of a cat contracting toxoplasmosis.
Home Remedies: None. Cats can contract toxoplasmosis through hunting birds and rodents, and eating undercooked food. Preventing outdoor exposure, hunting, and feeding raw food can reduce risk of a cat contracting toxoplasmosis.
What Is Toxoplasmosis?
Toxoplasmosis is a condition that develops following infection with the microscopic parasite Toxoplasma gondii. The parasite can affect all mammals, but cats particularly are important in the lifecycle and transmission of this parasite.
The fact that humans can also be infected, with very rare possible adverse consequences, means that this is a condition that can cause a great deal of concern to cat owners.
How Widespread Is Toxoplasmosis?
The parasite has a global distribution and is more common in tropical climates. Overall, it’s estimated that around 50% of the cats in the world have been infected by Toxoplasmosis at some stage in their lives. However, most cats show no detectable outward sign of Toxoplasma infection, so owners are unlikely to be aware that this has happened.
What Is the Life Cycle of the Toxoplasmosis Parasite?
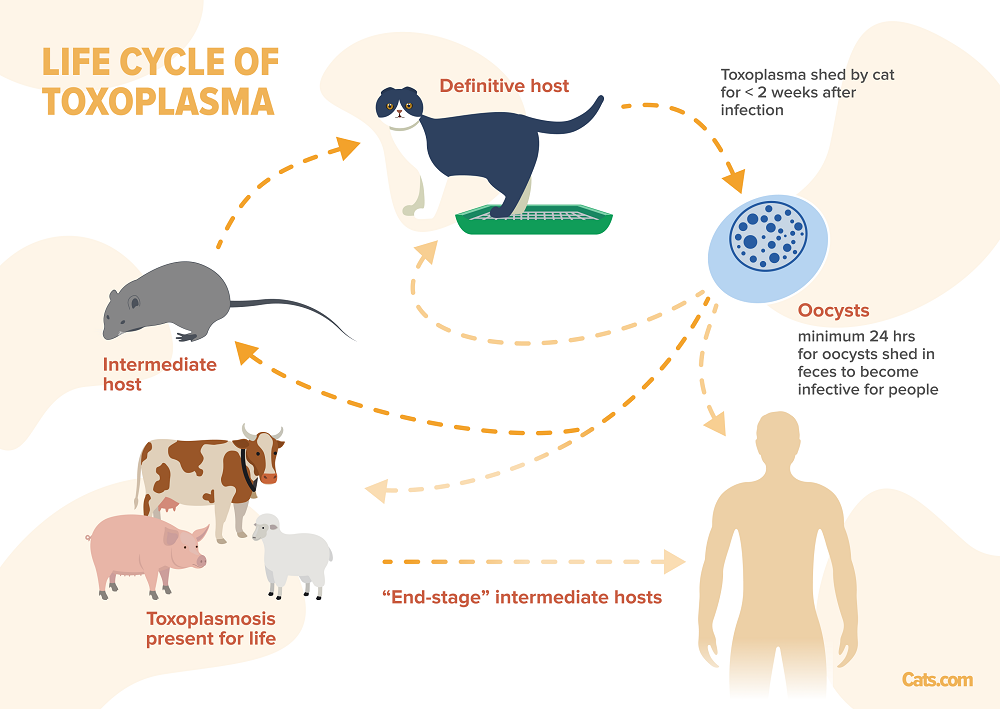
Life cycle of Toxoplasma
Toxoplasmosis gondii (T.Gondii) is a protozoon, single-celled parasite: this means that it is so tiny that it can only be seen under the microscope. The life cycle is complex, involving two types of host, so-called a “definitive” host and an “intermediate” host. The key difference between these types of hosts is as follows:
- The Toxoplasmosis parasite can produce eggs when they infect definitive hosts (cats)
- The Toxoplasmosis parasite cannot produce eggs when they infect intermediate hosts (all other animals), but they produce tissue cysts instead.
Cats (wild cats and domestic cats, including pet cats and stray cats) are the only animals that can be definitive hosts, so Toxoplasmosis organism can only produce eggs (known as “oocysts”) when they are inside a cat’s body.
All other warm-blooded animals can be intermediate hosts, including humans, and also including many species that provide food for cats, from farmed animals like cattle, sheep, poultry and pigs, to small animals like voles, mice, and birds to shellfish like oysters and mussels.
The toxoplasmosis parasite cannot produce eggs when they are inside intermediate hosts; instead, the parasite forms microscopic cysts in the animal’s tissues (muscles and organs), and these tissue cysts (known as zoitocysts) can infect other animals if the meat is eaten while raw. Zoitocysts remain in the host for the entire lifetime of the animal and remain infectious to any creature that consumes the animal. The zoitocyst is like a capsule, and it contains the active version of the toxoplasma parasite inside the capsule, which are known as bradyzoites.
During the T. Gondii life cycle, individual parasites convert into various stages, with different names, including the bradyzoites (found in tissue cysts or zoitocysts), sporozoites (found in oocysts), as well as tachyzoites and merozoites. The details of these parasitic stages do not need to be known to understand how to control T.Gondii infection.
How Do Cats, Humans, and Other Species Get Infected?
Cats, humans, and other species can become infected with Toxoplasmosis either by ingesting oocysts from cat feces, or by ingesting zoitocysts by eating animal tissues. Kittens can also become infected in the womb, by their mothers, and also via suckling their mother’s milk, but these routes of infection are rare. It is also possible for adult cats and humans to become infected after drinking unpasteurised milk from an infected cow or goat.
Cooking meat kills the zoitocysts, so infection is more common in outdoor cats that are hunters, in cats that are fed raw meat (the cooking involved in creating commercial cat food kills the parasite), and in humans who eat fresh, undercooked meat (the parasite is more common in humans in cultures that enjoy eating meat that has not been cooked so thoroughly e.g. France). Freezing meat also significantly reduces the risk of any zoitocysts being infectious.
How Do Infected Cats Pass On Toxoplasmosis Infection?
Immediately after cats have become infected, they shed oocysts in high numbers in their faeces for around two weeks. Once the two weeks are up, the cat’s immune response deals with the parasite, and oocysts are no longer shed in the faeces.
This is a key point: a cat that is “positive” for Toxoplamosis is actually unlikely to be shedding oocysts. It is only in the very early stage—for 14 days after initial infection—that the cat is infectious.
Importantly, oocysts that are passed in a cat’s faeces are not immediately infectious to other animals: a process called “sporulation” must take place, and this takes between one and five days.
The significance of this fact is that fresh cat faeces is unlikely to be infectious to humans, while “old” cat faeces may be infectious.
For this reason, humans who may be susceptible to adverse effects from Toxoplasmosis should avoid contact with “old” cat faeces (e.g. they should not clean out litter boxes).
Oocysts are tough, and can survive in the environment for many months, long after the faeces that originally carried them has dispersed.
So oocysts can be present in soil if a cat has passed faeces in the soil and buried it. If any other animal ingests these oocysts, they will hatch out when in their new host’s intestines, then the infection will spread from there to the bloodstream, and then to the rest of the body, creating new zoitocysts wherever they settle.
Symptoms of Toxoplasmosis in Cats

Because “old” faeces—that which has been sitting out for a day or more—is more likely to shed the oocysts that cause toxoplasmosis, at-risk people should avoid scooping their cat’s litter box.
Most cats show no clinical signs of infection with Toxoplasmosis, but rarely, fever, loss of appetite, weight loss, and lethargy may be noticed, with a wide range of other possible signs depending on the part of the body affected. This can include lung disease, liver disease, muscle pain, inflammatory disease affecting the eyes and brain, and enlarged lymph nodes.
Symptoms of Toxoplasmosis in Humans
The main issue of concern with Toxoplasmosis to cat owners is the rare, but possible, impact on human health. Healthy people are generally able to cope well with Toxoplasmosis infection: their immune system effectively eliminates the parasite, with no signs, or perhaps just flu-like symptoms like a mild fever with enlarged lymph nodes.
However, some sectors of the human population are regarded as being at high risk from more severe consequences from Toxoplasmosis.
This is because their immune systems are not able to deal with the parasite effectively. High risk groups include babies, young children, elderly people, and any immunocompromised people, either due to disease, or due to chemotherapy. Pregnant women are also high risk because of the risk to their unborn baby in the womb.
In these high-risk groups, the possible consequences of Toxoplasmosis infection include inflammation of the brain, nervous system and eyes, as well as abortion, stillbirth, and birth defects.
These potential serious consequences explain why it’s so important to understand Toxoplasmosis and to take steps to ensure that nobody is placed at risk.
How Common Is Toxoplasmosis in Cats?
Globally, around 50% of the cat population has been exposed to Toxoplasmosis at some stage, but again, it is important to remember that cats are only infectious during the immediate two week period after they have been infected.
So the percentage of cats that are actively infectious is far, far lower, and while it is impossible to calculate accurately, it’s more likely to be less 0.1% (i.e. less than one in a thousand cats). Clinical disease in cats caused by Toxoplasmosis is exceptionally rare as well.
How Common Is Toxoplasmosis in Humans?
There is significant geographic variation in the rates of human infection with Toxoplasmosis. Studies of antibodies to Toxoplasmosis have shown that in the UK, 20-30 percent of people have been exposed to the parasite at some stage, while in France and Germany, 80 percent of the population has evidence of exposure, and in the United States, according to the CDC website, this figure is around 12%.
The most worrying threat of Toxoplasmosis is the risk of abortion or birth defects when pregnant women become infected.
It’s estimated that in 20-50% of pregnant women who become infected while pregnant, there are adverse consequences.
Importantly, if a woman has been infected with Toxoplasmosis prior to pregnancy, her immune system will develop antibodies, and if she is exposed again to the parasite during pregnancy, there is no risk to her unborn baby. The only risk is to the babies of pregnant women who are exposed to Toxoplasmosis for the first time during pregnancy.
Does Owning a Cat Increase the Risk of a Person Picking Up Toxoplasmosis?
Studies have shown that, unexpectedly perhaps, contact with cats does not increase the risk of Toxoplasmosis infection in humans.
As stated above, cats only shed Toxoplasmosis eggs during the two weeks after initial infection, so while it is common for cats to be “positive” for Toxoplasmosis, it is exceptionally rare for cats to be actively infectious to humans.
Most humans are infected by eating raw or undercooked meat (which is probably why the infection is more common in France and Germany). The two risk areas that cat owners should address are pregnant women handling cat litter trays, and young children playing in gardens or sandboxes and handling soil or sand that may have been contaminated with infected cat faeces at some stage in the past.
Diagnosis of Toxoplasmosis

If you suspect that your cat may have toxoplasmosis, your veterinarian can help you with a diagnosis.
If you suspect that your cat may have Toxoplasmosis (based on the signs listed above), you should visit your local DVM veterinarian, where the following steps may be taken.
1. Detailed History Taking
Your vet will discuss every aspect of your cat’s life and health care: for example, Toxoplasmosis is more common in cats that are hunters, and cats that remain indoors all the time are far less likely to become infected. Cats that are FIV positive may be more likely to show signs as their immune system is compromised.
2. Physical Examination
Your veterinarian will check your cat over carefully, noting any physical signs of illness.
3. Routine Blood Tests
The usual blood tests, including haematology and biochemistry profiles, will give guidance on whether any particular systems are involved, and on how your cat’s immune system is reacting.
4. Specialised Blood Tests
A number of different serum titres for antibodies against Toxoplasma gondii are available, but importantly, these only indicate evidence of past exposure to the organism.
Careful assessment of different types of antibody, along with repeated samples to measure changing trends, may be helpful towards identifying active infections but expert interpretation of results is always needed. Your veterinarian will work with local centers for disease control and prevention to give you the best possible advice on this.
5. Faecal Tests
If a cat is actively shedding oocytes, these may be detected in the faeces, but this is rarely identified.
6. Histopathology
The tissue cysts (zoitocysts) may be seen in samples collected by biopsy.
7. Polymerase Chain Reaction (PCR) Assay
PCR assay can be carried out on faeces, biopsy samples, cerebrospinal fluid (CSF), and respiratory secretions. This is a sensitive test that identifies specific DNA evidence of Toxoplasmosis.
How Much Does a Cat Toxoplasmosis Test Cost?
You should ask your veterinarian about the costs of such tests, but they are likely to be somewhere between $50 and $200 depending on which specific test is being undertaken.
Treatment for Toxoplasmosis
Most cats do not need treatment for Toxoplasmosis: their immune system deals with the infection effectively.
Cats that fall ill because of Toxoplasmosis may be treated with a number of different medications, including clindamycin, trimethoprim-sulfonamide, pyrimethamine, ponazuril, and toltrazuril.
These are prescription-only drugs, so must only be given under strict veterinary supervision. Some are off-label, meaning that they do not have a specific licence to be used to treat Toxoplasmosis, which is another reason why they need veterinary guidance,
Tips for Preventing Toxoplasmosis Transmission

While most people can be infected with toxoplasmosis and only experience mild symptoms, some people experience more severe consequences. At-risk groups include babies, young children, elderly people, and those with compromised immune systems. Because unborn babies are at high risk, pregnant women should be very careful to avoid infection.
If you want to minimise the risk of your cat picking up Toxoplasmosis, keep them indoors, and only feed them cooked or processed meat.
Humans should be aware of the risk factors so that they know if they are potentially more vulnerable to ill effects from Toxoplasmosis infection.
This includes babies, young children, elderly people, and anyone with a suppressed immune system, either due to disease or due to chemotherapy.
Pregnant women are also high risk because of the risk to their unborn baby in the womb. People in these groups should take specific steps that include good hygiene around cats as well as caution around uncooked meat in the kitchen and dining room.
Here are a few ways to avoid infection with cat-related Toxoplasmosis:
- Avoid handling cat litter boxes, and avoid all contact with cat faeces.
- Clean the cat’s litter box regularly with detergent and hot water
- Dispose of cat litter safely e.g. sealed in a plastic bag and placed in the domestic trash
- Empty cat litter trays daily so if oocysts happened to be in the cat faeces, they would not be infective (as it takes several days for this to happen)
- Avoid handling soil that may have been contaminated with infected cat faeces at some stage in the past
- Wash fruit and vegetables carefully to remove all traces of soil
- Do not eat unwashed fruits
- Wear gloves and wash hands after gardening.
Here are ways to avoid meat-related Toxoplasmosis infection:
- Clean and wash all food preparation surfaces (including cutting boards) and utensils before and after use
- Cook all meat thoroughly to kill any tissue cysts
- Consider freezing fresh meat, then thawing it before cooking, as this makes tissue cysts less infectious
- Avoid eating raw shellfish (oysters, clams or mussels)
Conclusion
Toxoplasmosis is a complex microscopic parasite that rarely can cause serious disease in cats and humans.
The risk of cat owners developing toxoplasmosis is no higher than non-cat owners. However you should be aware of how the parasite is spread, and if you are in a vulnerable group as listed above, you should take simple steps to minimise further the very small risk of picking up the parasite.








Thankyou for your vet advise. Your report says that 50 percent of cats may have toxoplasmosis. I didn’t see any disclosure, that bloated abdomen would be one of the toxoplasmosis symptoms. My cat did have diarhea briefly in the beginning of ownership, but I thought it might be the corn meal base cat food. But at anyrate my cat has a bloated stomach and abdomen. that has been consistant since owned the cat. I thought it was being overweight. Cats health energy wise is very strong and active, no dessication. No growth on hair skin area. No fever, as far as i know. Don’t have a rectal thermometer, but that might be dangerous in exposing myself to the anal feces area. Don’t know. Could you please comment on the bloated stomach abdomen concerns I have with my cat. My cat was a kitten when I got her. She is about 23 weeks old. Her name is zooma because she zooms around alot. Very active cat. What do you think? I heard the toxoplasmosis antibody would tell me has the antigen surface on the gondhii parasite that the antibodies react to, IgM and IgG. PCR would only identify the present qualitative of the parasite, but not if it is active. CBC WITH differential, and giemsa wright stain, and methylene blue, would ID OTHER bacterial infection. C & S culture and sensitivity for bacteria gram negative gram positive might pickup something on lab test if use thioglycolate broth to culture it, before plating, and using a kirby baer disc test on blood agar plate. or MACANKEES plate. I know you said the two week is when it is transmissible. But, could cysts be picked up on differential blood plasma smear on feathered slide with cover slip at 100 or 200 magnification. Would the T cell count go up or down in slide chamber count. Thanks again ahead of time for your comments.
Sincerely Robert Fife
[email protected]
There is a long, long list of possible causes of bloated abdomen in cats, and the only way to find out would be to do tests including bloods, xrays and ultrasound. It is very unlikely to be toxoplasmosis. It is likely to be very difficult to see cysts on a blood plasma sphere, and the impact on the T cell count would be difficult to predict.
Sorry that I cannot be more helpful.
Pete