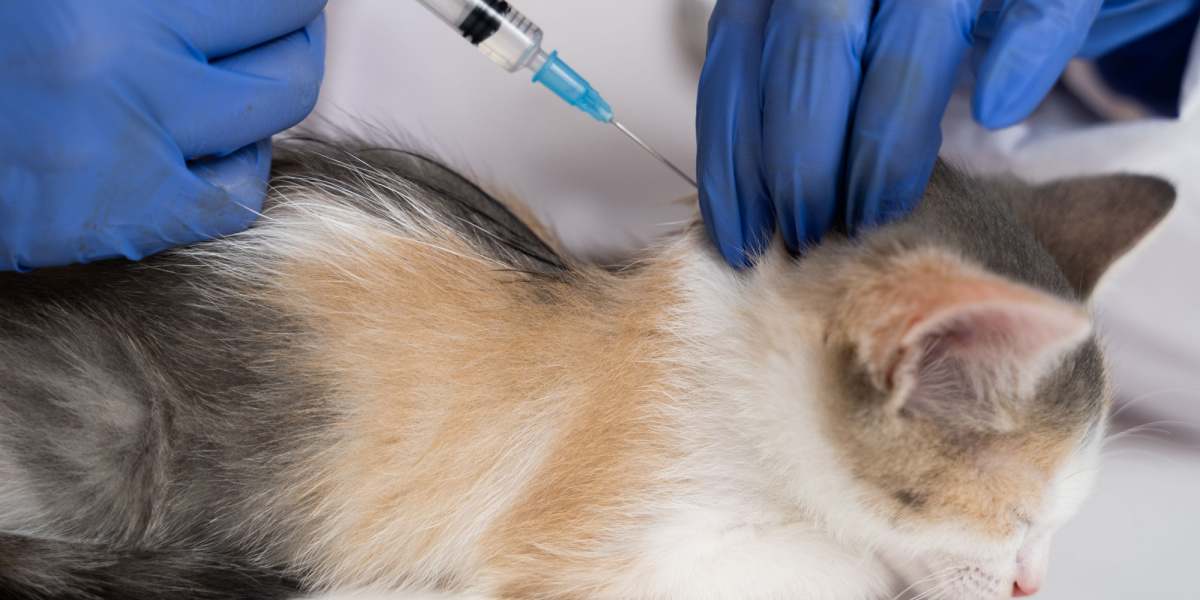
In this article, we’ll delve into the world of Feline Injection Site Sarcomas (FISS), a rare but concerning aspect of feline health. These tumors can develop at vaccination sites, emphasizing the significance of precise vaccination practices.
How Common Is Feline Injection-Site Sarcoma?
Feline injection-site sarcomas are hard to talk about. They are also (thankfully) quite rare, with only one in 1000 to one in 10 000 cats affected with this disease.
Having said this, being rare is not a comfort if your cat is the wrong number in the statistic. The cause of an injection-site sarcoma ( previously known as a vaccine-associated sarcoma) is multifactorial, but we can start with vaccines.
Some vaccines work by causing inflammation at the site, which will stimulate the immune system. These are called adjuvanted vaccines. The adjuvant serves a purpose, but in some cats, the inflammation at the site can cause the inflammatory cells to transform into cancer cells over time.
These cells can form a tumour called a fibrosarcoma. There are other causes of inflammation that can lead to a sarcoma. It is likely that cats that develop fibrosarcomas at injections sites are genetically predisposed to developing cancer.
The cancer that develops at injection sites is called fibrosarcoma. It is an extremely invasive form of cancer. This tumour causes most of its problems by being locally aggressive.
There is the tumour that you can see and feel and, surrounding this, there are microscopic cancer cells that invade the surrounding tissues. If only the mass is removed without taking a wide margin of normal tissues surrounding the mass, it will definitely recur and, often, the recurrent tumour is more aggressive than the original tumour.
This tumour can also spread or metastasize to other sites, but this is usually late in the course of the disease, with a metastatic rate of ~20%. The most common treatment for this type of cancer is surgery and the currently recommended margins of normal tissue to take around the tumour are 5cm around the mass and two layers of muscle underneath the mass.
This is a very big area and a big surgery for a patient the size of a cat. In large tumours or sites that are not amenable to surgery, these margins may not be possible and a combination of surgery and radiation may be recommended.
Decreasing risk, vaccine site placement, early detection, diagnosis and treatment are the keys to ensuring a good outcome if your cat is unfortunate enough to develop an injection-site sarcoma.
Decreasing Risk
It is important that your cat is vaccinated in order to keep them and your family healthy. Rabies is a serious risk to animal and human health and it is critical to ensure that your cat is vaccinated. So not vaccinating your cat is not a good option.
However, you should work with your veterinarian to tailor the vaccine protocol to suit your cat’s risk levels and lifestyle. There are nonadjuvanted vaccines for rabies that may decrease the risk of developing this tumour (because they have decreased inflammation around the injection site).
Nonadjuvanted rabies vaccines are more expensive, but, in my opinion, are worth the additional expense to lower the risk of developing a sarcoma.
Vaccine Site Placement
The current recommendations for vaccine sites in cats are outlined in the American Association of Feline Practitioners Vaccine Guidelines. They recommend that vaccinations should be given to cats below the elbow or knee.
This will likely look very different to what you are used to when you take your cat in for vaccination. The reason for this recommendation is that if your cat develops an injection-site sarcoma, the most successful treatment will be via limb amputation.
This is not something that we like to think about, but this option can be life saving. In the past (and unfortunately the present) vaccine sites can include the area between the shoulders and the hip or flank area. These sites can result in a tumour location that is very difficult to manage, with an inability to remove the mass in some cases or a radical surgery such as a body wall or hemipelvectomy (removing a portion of the pelvis and the limb) being required for successful removal.
There is one published study on vaccination in the tail, that did have an immune response in 95% of cats. I have vaccinated my own cat in the tail, but it is not common. If this site is chosen, it often requires shaving the tail and needs to be done in the lower half of the tail so that removal of the tail with 5cm margins would be feasible if required.
Early Detection

Early detection of injection site sarcomas is key to the successful treatment of this condition.
Like many cancers in animals and people, early detection can be the key to successful treatment. It is important to monitor your cat for skin masses everywhere, but to pay particular attention to the vaccine sites.
It is relatively common to have a small lump at a vaccine site in the weeks that follow vaccination, so don’t panic if you feel this. However, if the mass is persistent for more than a month, firm or growing, some attention is required.
A sarcoma can grow months to years after vaccination, so any masses at previous injection sites should be investigated. Although a fine needle aspirate (putting a needle into the mass and taking a sample of the cells to send to the lab for cytology) is generally recommended as the first step in investigating any skin mass, this tumour type is different.
The cytology test can be misleading in this case, as it can be hard to distinguish between inflammation and tumour cells. The best test, if an injection site sarcoma is suspected, is a tissue biopsy.
The biopsy is not the same as removing the mass. A small portion of the mass will be removed, but the mass will remain in place until a diagnosis is reached so that a definitive surgery can be planned.
Treatment Planning
If an injection-site sarcoma is diagnosed with the biopsy, the next step is planning for treatment. This may involve blood tests to evaluate the overall health of your cat and staging tests to evaluate the tumour more carefully and to assess if there is any evidence of spread to the lungs.
In my patients, this is most often done with a CT scan of the chest to evaluate the lungs and of the affected area. If I am very suspicious of an injection-site sarcoma, I often do the CT scan and the biopsy at the same time as both require either very heavy sedation or a general anesthetic.
Treatment

Surgery is the most effective treatment for injection-site sarcoma.
The most effective treatment for injection-site sarcoma is surgery. If the vaccine site is below the elbow or the knee, limb amputation will provide the best outcome in most cases and this is the recommended treatment.
These surgeries are often considered referral surgeries and referral to a board-certified veterinary surgeon should be discussed prior to treatment. In tumours that are too large to achieve 5cm margins or in locations where this is not achievable, we may consider a combination of surgery and radiation.
Sometimes the radiation is given before surgery and sometimes surgery is done first . Unfortunately, the outcome with this combined therapy is not as good overall as in cases where the desired margins can be achieved.
Follow-up Care
Most cats will do very well after limb amputation if they are in good body condition. After surgery, the removed tissues are submitted to the lab to confirm the diagnosis and to assess the margins of excision.
This is how we can assess if all the tumour cells have been removed. The pathologist will look along the cut edges of the removed tissues and report. If no cancer cells are seen microscopically within 5mm of the margins or cut edges, the tumour will be considered to be completely removed (clean margins).
In general, if the margins of excision are clean, no further treatment will be recommended. Chemotherapy is not typically recommended for this disease as the rate of spread to the lungs is relatively low (20%) but there can be exceptions to this.
Radiation therapy is typically recommended in cases where there is evidence of incomplete margins. Continued vaccination of cats that have had this disease is generally not recommended.
Conclusions
With a vaccine protocol that is tailored to your pet, appropriate vaccine-site placement, early detection, and appropriate surgical margins, successful outcomes are possible with this highly aggressive form of cancer.
Frequently Asked Questions
How long do cats live with injection site sarcoma?
This will depend almost entirely on the success of surgical treatment. The median survival time for cats that have had surgery with the wide margins described is 901 days, with a big different observed between cats with complete margins (1461 days) versus incomplete margins (499 days). The size and location of the tumour will dictate the ability to achieve clean margins, so early detection and placement of vaccines on the lower limb have the potential to have a big impact on survival in these cats.
How common is injection site sarcoma in cats?
This disease occurs in 1 in 1000 to 1 in 10 000 cats
What is injection site sarcoma in cats?
This is a cancer that forms at injection sites that are most commonly associated with vaccination. It is associated with a transformation of inflammatory cells into cancer cells.
Can vaccines cause lumps?
Many vaccines can cause a lump or mass at the site of vaccination. This is not something to worry about unless it is persistent or growing. If you notice a lump at a previous vaccination site, contact your veterinarian.
-
Stone AE, Brummet GO, Carozza EM, Kass PH, Petersen EP, Sykes J, Westman ME. 2020 AAHA/AAFP Feline Vaccination Guidelines. J Feline Med Surg. 2020 Sep;22(9):813-830. doi: 10.1177/1098612X20941784. PMID: 32845224.
-
Phelps HA, Kuntz CA, Milner RJ, Powers BE, Bacon NJ. Radical excision with five-centimeter margins for treatment of feline injection-site sarcomas: 91 cases (1998-2002). J Am Vet Med Assoc. 2011 Jul 1;239(1):97-106. doi: 10.2460/javma.239.1.97. PMID: 21718202.
-
Kirpensteijn J. Feline injection site-associated sarcoma: Is it a reason to critically evaluate our vaccination policies? Vet Microbiol. 2006 Oct 5;117(1):59-65. doi: 10.1016/j.vetmic.2006.04.010. PMID: 16769184.
-
Hartmann K, Day MJ, Thiry E, Lloret A, Frymus T, Addie D, Boucraut-Baralon C, Egberink H, Gruffydd-Jones T, Horzinek MC, Hosie MJ, Lutz H, Marsilio F, Pennisi MG, Radford AD, Truyen U, Möstl K; European Advisory Board on Cat Diseases. Feline injection-site sarcoma: ABCD guidelines on prevention and management. J Feline Med Surg. 2015 Jul;17(7):606-13. doi: 10.1177/1098612X15588451. PMID: 26101312.